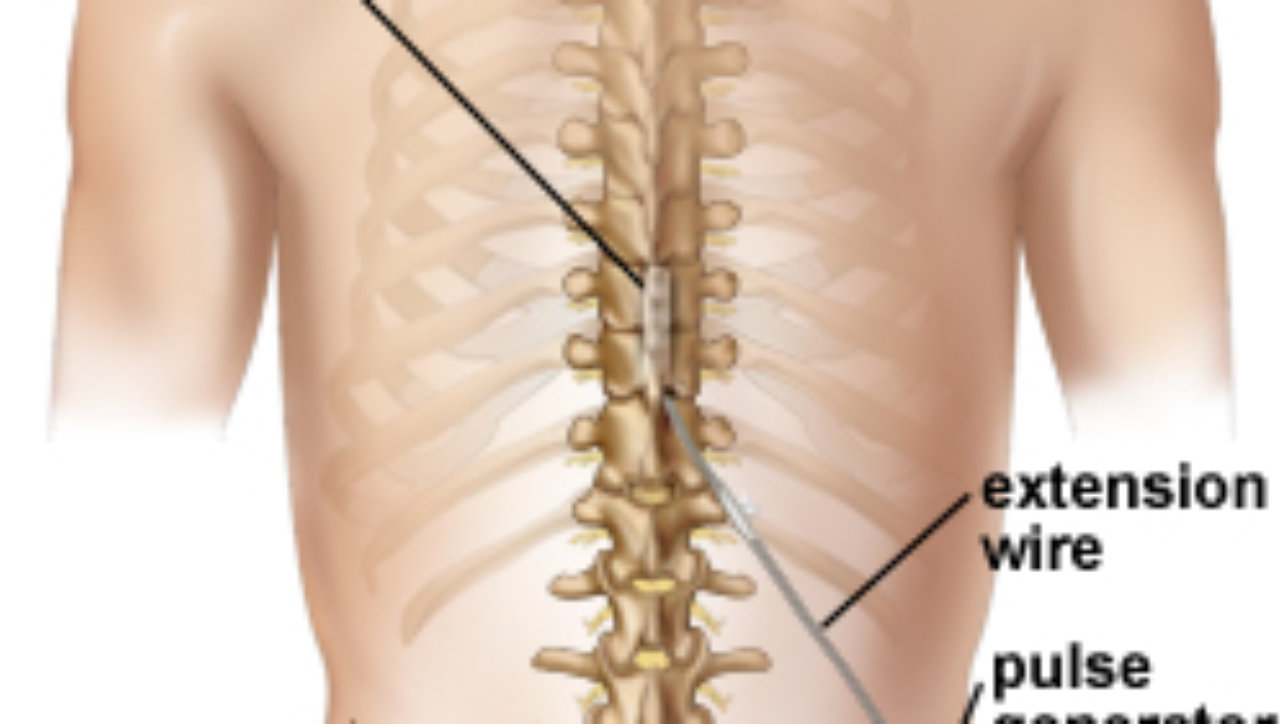
Spinal cord stimulation is a therapy that masks pain signals before they reach the brain. A small device, similar to a pacemaker, is implanted in the body to deliver electrical pulses to the spinal cord. It helps patients better manage their chronic pain symptoms and decrease the use of opioid medications. It may be an option if you suffer chronic back, leg or arm pain and have not found relief with other therapies.
Read more
Cancer Pain Management
What is pain management?
Pain management is a branch of medicine focused on reducing pain and improving quality of life through an integrative approach to care. Pain management is particularly important for cancer patients, considering one in three patients continues to experience pain after treatment.
If you have pain, the severity and prevalence of your pain may depend on many factors, including the type and stage of your cancer, your treatment plan and your tolerance for pain. You may experience pain from the cancer itself, or as a side effect of cancer treatment. Those with advanced cancer are most likely to have severe pain. Cancer pain may result from:
- A tumor putting pressure on tissues, bones, nerves or organs
- Poor blood circulation because the cancer has blocked blood vessels
- Blockage of an organ or tube in the body, such as the kidneys or bladder
- Side effects of surgery, radiation therapy, chemotherapy or other cancer treatments
- Metastasis, or cancer cells that have spread to other locations in the body
- Pain that is completely independent from cancer or cancer treatment (e.g., headaches, backaches, muscle strains, arthritis or other common pains)
Pain management may improve quality of life at any stage of cancer, so managing your pain is our priority. Our experienced pain management team cares for you throughout your treatment, to help reduce your pain and help you get comfortable. We use a variety of modalities to treat and control pain, including:
- Prescription medications
- Implanted pain pumps
- Nerve block therapies
- Physical therapy
- Acupuncture and auriculotherapy
- Massage therapy
- Relaxation techniques and guided imagery
- Chiropractic treatmen
Experienced care team
The team approach to care is critical for pain management. Our team of pain management providers work with your oncologist and other members of your care team to manage your pain related to cancer or its treatment. In addition to medication, your pain management regimen may include one or more of our supportive care services, such as:
- Naturopathic medicine, which uses natural therapies to help you combat pain, as well as reduce the hormonal side effects that may accompany cancer treatment
- Oncology rehabilitation, which plays a key role in pain management by using a variety of physical therapy and other techniques to improve mobility and trigger the release of endorphins, which is the body’s natural defense against pain
- The mind-body medicine team, which is available to teach you relaxation tools to help you manage pain, and to reduce the anxiety and fatigue related to cancer or its treatment
For patients staying at the hospital, the pain management team is available for referrals. During these visits, pain management practitioners thoroughly evaluate your pain level and assess how your pain management approach is working. Based on their evaluation, these clinicians will make modifications to your treatment plan as needed.
Personalized treatment approach
The pain symptoms you experience are unique to you, which is why we tailor your pain management plan to your individual case. Pain itself may be dull, achy or sharp. It may occur frequently or once in a while, and it may be mild, moderate or severe. The pain you experience may depend on your cancer type and stage, how much the cancer has spread, and how sensitive you are to pain (your pain tolerance). Whatever type of pain you experience, we want to treat it early to prevent it from worsening.
Managing side effects
Some prescription medicines used to treat pain have side effects, including nausea, vomiting, itching, constipation and drowsiness. Your doctor may change the dosage, the time the medicine is taken or the medicine itself to see if you experience fewer side effects. In addition, our supportive care practitioners will work together to help you manage side effects that you experience with pain management. We offer nutrition therapy, naturopathic medicine, mind-body medicine and other services.
Spine Disk Alignment
What Are Spinal Disk Problems?
Anybody who has experienced a damaged spinal disk understands how painful it is. Every movement seems to make it worse.
This pain is a warning signal that you should heed. If you take appropriate action, the discomfort usually stops, and the problem can be corrected.
Spinal disks are rubbery pads between the vertebrae, the specialized bones that make up the spinal column. Doctors call them intervertebral disks. Each disk is a flat, circular capsule about an inch in diameter and one-quarter inch thick. They have a tough, fibrous, outer membrane (the annulus fibrosus), and an elastic core (the nucleus pulposus).
The disks are firmly embedded between the vertebrae and are held in place by the ligaments connecting the spinal bones and the surrounding sheaths of muscle. There is really little, if any, room for disks to slip or move. The points on which the vertebrae turn and move are called facet joints, which stick out like arched wings on either side of the rear part of the vertebrae. These facet joints are separate from the discs and keep the vertebrae from bending or twisting excessively, which could damage the spinal cord and the vital network of nerves that runs through the center of the spinal canal formed by the stack of vertebra.
The disk is sometimes described as a shock absorber for the spine, which makes it sound more flexible or pliable than it really is. While the disks do separate the vertebrae and keep them from rubbing together, they are far from spring-like. In children, they are gel- or fluid-filled sacs, but they begin to solidify as part of the normal aging process. By early adulthood, the blood supply to the disk has stopped, the soft inner material has begun to harden, and the disk is less elastic. By middle age, the disks are tough and quite unyielding, with the consistency of a piece of hard rubber. These changes related to aging make the outer protective lining weaker and the disks more prone to injury.
Understanding Spinal Disk Problems — Herniated Disk
Under stress, a disk’s inner material may swell, pushing through its tough outer membrane. The entire disk can become distorted or bulge in spots. With an injury, all or part of the core material may protrude through the outer casing at a weak spot, pressing against surrounding nerves. If further activity or injury causes the membrane to rupture or tear, the disk material may further extrude, causing pressure on the spinal cord or the nerves that radiate from it. This may result in extreme pain. In the beginning, there may be spasms in the back or neck which will greatly limit your movement. If nerves are affected, you may develop pain that moves into a leg or an arm.
The vast majority of disk injuries occur in the lumbar region of the lower back. Only 10% of these injuries affect the upper spine. Not all herniated disks press on nerves, however, and it is entirely possible to have deformed disks without any pain or discomfort.
Herniated disks are most common in men and women ages 30 to 50, although they also occur in active children and young adults. Older people, whose disks no longer have fluid cores, are much less likely to encounter the problem. People who do regular, moderate exercise are much less likely to suffer from disk problems than sedentary adults. People who exercise tend to stay flexible considerably longer. Maintaining a normal body weight is also important in preventing back problems.
What Causes a Herniated Disk?
Although a violent injury can damage a disk, problems with disks are often brought on by the normal aging process or by everyday activities, such as lifting heavy objects the wrong way, stretching too hard during a tennis volley, or slipping and falling on an icy sidewalk. Any such event can cause the fibrous outer covering of the disk to break or distort to the point that it presses on a spinal nerve, especially if disk material extrudes. Sometimes, a disk swells, tears, or degenerates without any apparent cause.
Understanding Spinal Disk Problems — Degenerative Disk Disease
Disk problems are sometimes lumped together under the term degenerative disk disease. Change in the condition of the disk is a natural result of aging. This is part of our gradual loss of flexibility as we grow older.
But disk degeneration is far more serious in some people than in others. Severe cases may be the result of a deficiency in collagen, the material that makes up cartilage. Poor muscle tone, poor posture, and obesity also put excessive strain on the spine and the ligaments that hold the disks in place.
Nerve Block Injections
Pain Management and Nerve Blocks
Often a group of nerves, called a plexus or ganglion, that causes pain to a specific organ or body region can be blocked with the injection of medication into a specific area of the body. The injection of this nerve-numbing substance is called a nerve block.
How Are Nerve Blocks Used?
There are different kinds of nerve blocks used for various purposes.
- Therapeutic nerve blocks are used to treat painful conditions. Such nerve blocks contain local anesthetic that can be used to control acute pain.
- Diagnostic nerve blocks are used to determine sources of pain. These blocks typically contain an anesthetic with a known duration of relief.
- Prognostic nerve blocks predict the outcomes of given treatments. For example, a nerve block may be performed to determine if more permanent treatments (such as surgery) would be successful in treating pain.
- Preemptive nerve blocks are meant to prevent subsequent pain from a procedure that can cause problems including phantom limb pain.
- Nerve blocks can be used, in some cases, to avoid surgery.
Types of Nerve Blocks
Various areas of pain require different nerve block types. Below are a few of the available nerve blocks and some parts of the body where they are used.
- Trigeminal nerve blocks (face)
- Ophthalmic nerve block (eyelids and scalp)
- Supraorbital nerve block (forehead)
- Maxillary nerve block (upper jaw)
- Sphenopalatine nerve block (nose and palate)
- Cervical epidural, thoracic epidural, and lumbar epidural block (neck and back)
- Cervical plexus block and cervical paravertebral block (shoulder and upper neck)
- Brachial plexus block, elbow block, and wrist block (shoulder/arm/hand, elbow, and wrist)
- Subarachnoid block and celiac plexus block (abdomen and pelvis)
Other Nerve Blocks
Other types of nerve blocks include:
- Sympathetic nerve block: A sympathetic nerve block is one that is performed to determine if there is damage to the sympathetic nerve chain. This is a network of nerves extending the length of the spine. These nerves control some of the involuntary functions of the body, such as opening and narrowing blood vessels.
- Stellate ganglion block: This is a type of sympathetic nerve block performed to determine if there is damage to the sympathetic nerve chain supplying the head, neck, chest, or arms and if it is the source of pain in those areas. Although used mainly as a diagnostic block, the stellate ganglion block may provide pain relief in excess of the duration of the anesthetic.
- Facet joint block: Also known as a zygapophysial joint block, the facet joint block is performed to determine whether a facet joint is a source of pain. Facet joints are located on the back of the spine, where one vertebra slightly overlaps another. These joints guide and restrict the spines movement.
Side Effects and Risks of Nerve Blocks
Nerve blocks do have risks and side effects. They include:
- Elevated blood sugars
- Rash
- Itching
- Weight gain
- Extra energy
- Soreness at the site of injection
- Bleeding
- Death (in rare cases)
Although many kinds of nerve blocks exist, this treatment cannot always be used. If your pain isn’t related to pain in a single or small group of nerves, nerve blocks may not be right for you. Your doctor can advise you as to whether this treatment is appropriate for you.
Radiofrequency ablation FAQ
Radiofrequency ablation (or RFA) is a procedure used to reduce pain. An electrical current produced by a radio wave is used to heat up a small area of nerve tissue, thereby decreasing pain signals from that specific area.
Which Conditions Are Treated With Radiofrequency Ablation?
RFA can be used to help patients with chronic (long-lasting) low-back and neck pain and pain related to the degeneration of joints from arthritis. Read more